The FDA approval for the 9LA regimen is for any PD-L1 type, positive or negative, in non–small cell lung cancer. The duration of response was better for those who responded to treatment, and progression-free survival was better for the 9LA regimen compared with the chemotherapy.įor 9LA, the primary end point was overall survival compared with chemotherapy for all PD-L1 types. It was superior to chemotherapy, and it was superior for overall survival, progression-free survival, and overall response rate. In this trial, the 9LA regimen was positive. To prevent early progression, avoid long-duration toxicity from chemotherapy, then also provide the double immunotherapy for a chance for a higher number of immune responses that will give us a really long duration of benefit, a long-term benefit of 3, 4, and 5 years. That’s particularly a concern in patients who have a high tumor volume or are symptomatic from their cancer, so this regimen gave only 2 cycles of chemotherapy. The reason for the 2 cycles of chemotherapy is that with immunotherapy, sometimes we will see early progression. The experimental arm was nivolumab and low-dose ipilimumab regimen from CheckMate 227 plus 2 cycles of chemotherapy. CheckMate 9LA was a randomized phase 3 trial for all-histology lung cancer, and the control arm was standard histology-based chemotherapy. While CheckMate 227 was a long time coming and it took awhile to have approval for nivolumab and ipilimumab on the CheckMate 227 regimen, 9LA came on us all of a sudden. Ready, MD: I’m going to talk about CheckMate 9LA. Some propose that may be countering hyperprogression, but in any case we see the favorable early benefit from adding chemotherapy in that long-term tail with a dual-checkpoint blockade. We don’t see that crossing of the early curves, just 2 cycles of chemotherapy preventing benefit. 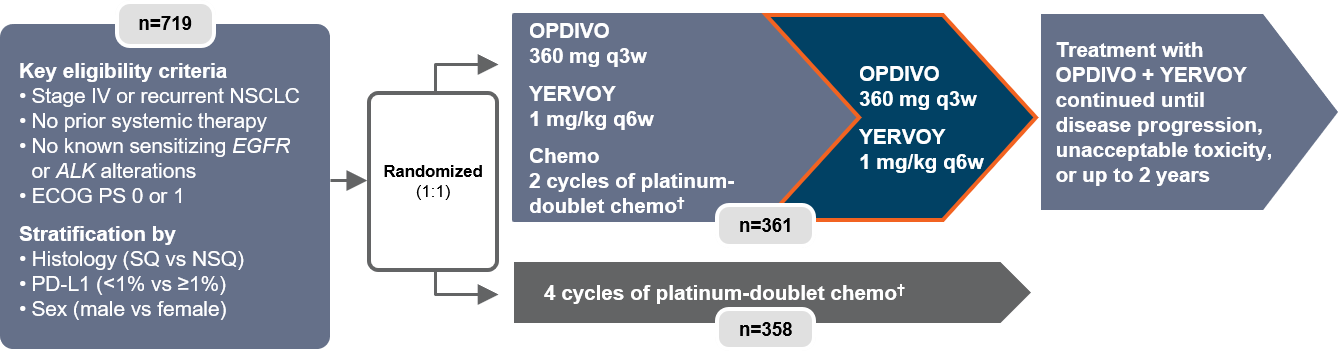
When we look at those Kaplan-Meier curves for PFS, and we don’t see that initial drop. We also saw the PFS benefit, 6.7 months with nivo-ipi –chemotherapy versus 5 months with chemotherapy alone with a hazard ratio of 0.68. One-year survival rates across PD-L1 subsets were 60% to 70%. In the PD-L1–high group, 0.66, which is remarkably similar across. If we look at the PD-L1–negative group, the survival hazard ratio was 0.62. The control arms didn’t necessarily underperform. In both squamous and nonsquamous histologies, really across PD-L1 subsets, the addition of nivo-ipi to 2 cycles of chemotherapy provided a clear benefit over chemotherapy alone. In the squamous, 14.5 months versus 9.1, hazard ratio of 0.62. Broken down by histology in the nonsquamous group, we saw 17-month OS versus 11.9, hazard ratio of 0.69. The 1-year survival rate was 63% compared with 47% with chemotherapy. Overall survival was 15.6 months versus 10.9 months with a hazard ratio of 0.66. Compared with chemotherapy alone, the chemotherapy–nivo-ipi approach did provide a survival benefit. Here it was about 40% PD-L1 negative, so you just want to keep those populations in mind when we look at absolute numbers. 
If you look at the PD-L1 breakdown, we would typically expect about a third negative, a third positive low, and a third positive high. About 30% were squamous, a little different from studies like KEYNOTE-024, where it was closer to 20%. Now, it’s important to look at the patient characteristics. When we look at the outcome from this phase 3 registrational trial, over 700 patients randomized, there was a survival benefit. Then, toward the cycles beyond the second round, to lean more on that dual-checkpoint blockade for durable benefit and for more meaningful duration of response. The rationale and strategy is to provide a means to get that initial rapid cytotoxic control, to avoid that initial drop in PFS to provide that benefit for patients with aggressive disease or high burden of disease and facilitate an initial response. The unique wrinkle here is that chemotherapy was given only with the first 2 cycles, not the first 4, and there was no indefinite maintenance chemotherapy. This is a combination of platinum doublet chemotherapy, histology specific, combined with dual-checkpoint blockade using the PD-1 inhibitor nivolumab and the CTLA4 inhibitor ipilimumab. This was the first time in my knowledge that we had approval of the drug before we see any of the data. Stephen Liu, MD: The CheckMate 9LA regimen is the most recent regimen that was added to our treatment arsenal.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
